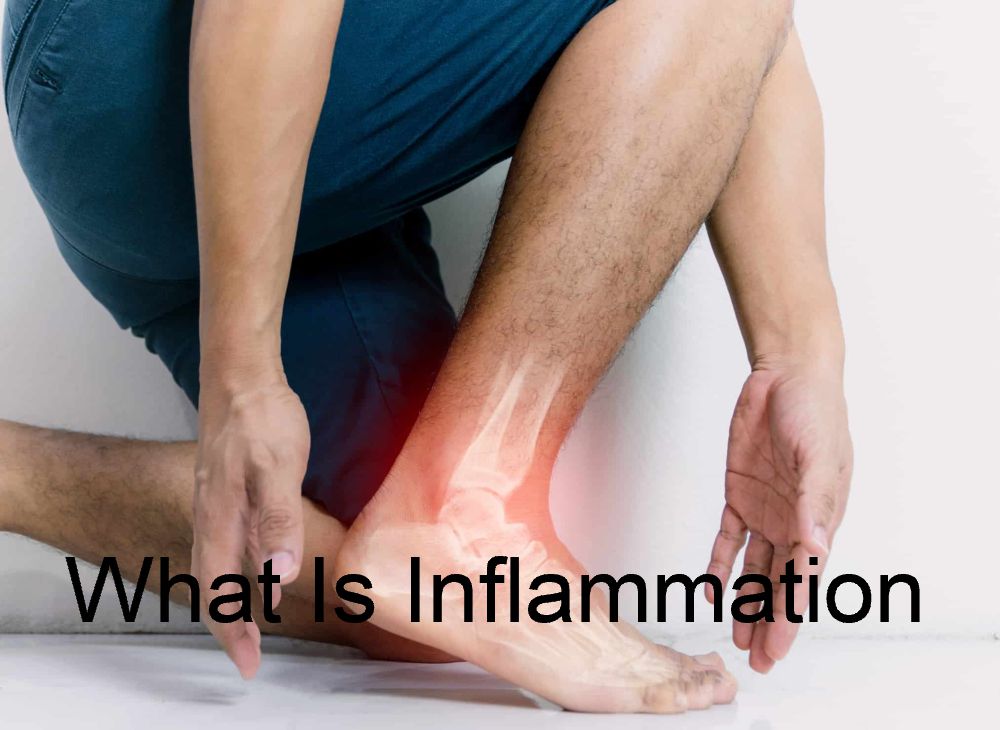
Osteoarthritis is a common condition that affects millions of people worldwide, causing joint pain and stiffness. It occurs when the cartilage that cushions the joints breaks down, leading to bone-on-bone contact and discomfort.

The symptoms of arthritis can vary from person to person but often include pain, stiffness, and limited mobility in the affected joints. Understanding the causes and symptoms is crucial for seeking appropriate treatment.
Treatment options range from lifestyle changes and physical therapy to medication and surgery, depending on the severity of the condition.
Key Takeaways
- Understanding osteoarthritis is crucial for managing its symptoms.
- Joint pain and stiffness are common symptoms.
- Cartilage breakdown is a primary cause.
- Treatment options vary based on the condition’s severity.
- Lifestyle changes can significantly impact symptom management.
What Is Osteoarthritis?
The term osteoarthritis refers to a condition characterized by the breakdown of cartilage in joints. This degenerative joint disease is the most common form of arthritis, affecting millions of people worldwide.
Definition of the Most Common Form of Arthritis
Osteoarthritis is primarily characterized by the deterioration of cartilage, which is the slippery tissue that covers the ends of bones where they form a joint. As cartilage breaks down, it leads to bone-on-bone contact, resulting in pain and stiffness.
How Osteoarthritis Affects Joints
Osteoarthritis affects joints by causing the cartilage to wear away, leading to bone spurs and inflammation. This can result in pain, stiffness, and reduced mobility in the affected joints. Commonly affected areas include the hands, knees, hips, and spine.
Prevalence and Impact
Osteoarthritis is a significant health concern due to its high prevalence and impact on quality of life. According to the Arthritis Foundation, osteoarthritis affects over 32.5 million adults in the United States alone.
| Prevalence | Impact |
|---|---|
| Over 32.5 million adults in the US | Reduced quality of life |
| Increasing with age | Significant healthcare costs |
| More common in women | Loss of productivity |
Understanding osteoarthritis is crucial for managing its symptoms and improving the quality of life for those affected.
The Science Behind Joint Damage
Understanding the science behind joint damage is crucial for comprehending osteoarthritis and its impact on joints. Osteoarthritis is a complex condition characterized by the deterioration of joint cartilage, leading to significant joint damage and discomfort.
Cartilage Breakdown Process
The cartilage breakdown process is a hallmark of osteoarthritis. Cartilage serves as a cushion between the bones, allowing for smooth movement. In osteoarthritis, this cartilage deteriorates, leading to bone-on-bone contact and pain. The breakdown is often a result of a combination of factors, including age, wear and tear, and genetic predisposition.
Bone Spurs Formation
Bone spurs, or osteophytes, are abnormal bone growths that form around the joints affected by osteoarthritis. These growths can cause additional pain and limit the range of motion. The formation of bone spurs is the body’s attempt to repair the damage by creating more bone, but it ultimately leads to further complications.
Inflammation in Osteoarthritis
Inflammation plays a significant role in the progression of osteoarthritis. While osteoarthritis is not primarily an inflammatory condition like rheumatoid arthritis, inflammation can occur, especially in the later stages. This inflammation can exacerbate the symptoms, leading to increased pain and swelling.
In conclusion, the science behind joint damage in osteoarthritis involves a complex interplay of cartilage breakdown, bone spurs formation, and inflammation. Understanding these mechanisms is crucial for developing effective treatment strategies.
Types of Osteoarthritis
Understanding the different types of osteoarthritis is crucial for effective management and treatment. Osteoarthritis is categorized into several types based on its causes, symptoms, and progression.
Primary Osteoarthritis
Primary osteoarthritis is the most common form, typically associated with aging and wear and tear on the joints. It often affects multiple joints and is characterized by a gradual degeneration of cartilage.
Secondary Osteoarthritis
Secondary osteoarthritis results from specific causes such as injury, infection, or another joint condition. It can occur at any age and may affect a single joint or multiple joints.
Common causes of secondary osteoarthritis include:
- Joint injuries or trauma
- Infections that damage the joint
- Other arthritic conditions like rheumatoid arthritis
Erosive Osteoarthritis
Erosive osteoarthritis is a more aggressive form, characterized by rapid progression and significant joint damage. It often affects the joints of the hands and can lead to deformity if not properly managed.
In summary, recognizing the type of osteoarthritis is essential for choosing the right treatment approach. Each type has distinct features and requires a tailored management plan to alleviate symptoms and improve quality of life.
Common Locations for Osteoarthritis
Osteoarthritis can affect various joints in the body, but some areas are more prone to this condition than others. The disease tends to target weight-bearing joints and those with high usage, leading to significant discomfort and mobility issues.
Knee Osteoarthritis
Knee osteoarthritis is one of the most common forms, often resulting from wear and tear over time. Symptoms include pain, stiffness, and reduced mobility. Factors such as obesity, previous injuries, and genetic predisposition can increase the risk.
Hip Osteoarthritis
Hip osteoarthritis affects the hip joint, causing pain and stiffness in the groin or thigh area. Activities like walking or climbing stairs can become challenging. The condition can be primary, related to aging, or secondary due to injury or developmental issues.
Hand and Finger Joints
Osteoarthritis in the hands and fingers can lead to pain, swelling, and deformity. It often affects the distal interphalangeal joints (DIP) and can result in the formation of Heberden’s nodes. This type of osteoarthritis is more common in women and can have a significant impact on daily activities.
Spine Osteoarthritis
Spine osteoarthritis can occur in both the cervical and lumbar regions, leading to pain, stiffness, and sometimes nerve compression. It can result from degenerative changes, trauma, or other factors. Management strategies often include physical therapy and lifestyle modifications.
Understanding the common locations for osteoarthritis is crucial for early diagnosis and effective management. By recognizing the symptoms and risk factors associated with different joints, individuals can seek appropriate medical care and adopt preventive measures to slow disease progression.
- Key areas affected:
- Knee
- Hip
- Hand and finger joints
- Spine
Each of these locations presents unique challenges and requires tailored approaches to treatment and management.
Recognizing Osteoarthritis Symptoms
Recognizing the signs of osteoarthritis can help individuals seek medical attention and improve their quality of life. Osteoarthritis symptoms can vary in severity and impact daily activities significantly.
Joint Pain and Stiffness
One of the primary symptoms of osteoarthritis is joint pain, which can range from mild to severe. This pain is often accompanied by stiffness, particularly after periods of rest or inactivity. For example, individuals might experience stiffness in the morning that eases as they move around.
Reduced Range of Motion
Osteoarthritis can lead to a reduced range of motion in the affected joints. This limitation can make everyday tasks challenging, such as bending, straightening, or rotating the joint. Regular exercise and physical therapy can help maintain flexibility.
Swelling and Tenderness
Swelling and tenderness around the joint are common symptoms of osteoarthritis. These occur due to inflammation and can be exacerbated by overuse or injury. Applying ice packs and elevating the affected limb can provide relief.
Grating Sensation and Bone Spurs
Some individuals with osteoarthritis may experience a grating sensation when moving the affected joint, known as crepitus. This is often due to the roughening of the cartilage surface. Additionally, bone spurs can form, further contributing to discomfort and limited mobility.
Understanding these symptoms is crucial for early diagnosis and effective management of osteoarthritis. If you’re experiencing any of these signs, it’s essential to consult with a healthcare professional for proper evaluation and treatment.
Causes and Risk Factors of Osteoarthritis
Understanding the causes and risk factors of osteoarthritis is crucial for effective prevention and management. Osteoarthritis is a complex condition influenced by a variety of factors.
Age-Related Wear and Tear
One of the primary risk factors for osteoarthritis is age. As people get older, the cartilage in their joints naturally deteriorates, making it more susceptible to damage. Age-related wear and tear is a significant contributor to the development of osteoarthritis.
Genetic Predisposition
Genetics also play a crucial role in the development of osteoarthritis. Individuals with a family history of osteoarthritis are more likely to develop the condition. Research has identified several genes that may contribute to the risk of osteoarthritis.
Joint Injuries and Overuse
Joint injuries, such as those sustained during sports or accidents, can significantly increase the risk of developing osteoarthritis. Similarly, repetitive strain on the joints due to overuse can also contribute to the condition.
Obesity and Weight-Bearing Joints
Obesity is another major risk factor, particularly for weight-bearing joints like the knees and hips. Excess weight puts additional strain on these joints, accelerating the wear and tear process.
| Risk Factor | Description | Impact on Osteoarthritis |
|---|---|---|
| Age | Natural deterioration of cartilage over time | Increased risk with age |
| Genetics | Family history and genetic predisposition | Higher likelihood with genetic factors |
| Joint Injuries | Trauma or overuse leading to joint damage | Increased risk of osteoarthritis |
| Obesity | Excess weight on weight-bearing joints | Accelerated wear and tear |
Osteoarthritis vs. Rheumatoid Arthritis
While both osteoarthritis and rheumatoid arthritis impact joints, their underlying causes and manifestations differ significantly. Osteoarthritis (OA) is primarily a degenerative joint disease resulting from wear and tear over time, whereas rheumatoid arthritis (RA) is an autoimmune disorder that causes the immune system to attack the lining of the joints.
Key Differences in Causes
The causes of OA and RA are distinct. OA is largely attributed to age-related wear and tear, genetics, and joint injuries. In contrast, RA is caused by an abnormal immune response, leading to inflammation and joint damage.
Contrasting Symptoms and Progression
Symptoms of OA typically include joint pain and stiffness, particularly after periods of rest or inactivity. RA, on the other hand, often presents with symmetrical joint pain, swelling, and stiffness, accompanied by systemic symptoms like fatigue and fever. The progression of OA is generally gradual, while RA can progress rapidly if left untreated.
Different Treatment Approaches
Treatment for OA focuses on managing pain and improving joint function through lifestyle modifications, physical therapy, and medications. RA treatment involves disease-modifying antirheumatic drugs (DMARDs) to slow disease progression, alongside pain management and lifestyle adjustments.
In summary, understanding the differences between OA and RA is crucial for effective management and treatment. While OA is a localized degenerative condition, RA is a systemic autoimmune disease requiring distinct therapeutic approaches.
When to See a Doctor
Knowing when to seek medical attention is crucial for managing osteoarthritis effectively. Recognizing the warning signs that require a doctor’s visit can help you address your symptoms promptly and prevent further joint damage.
Warning Signs That Require Medical Attention
If you’re experiencing any of the following symptoms, it’s time to schedule an appointment with your doctor:
- Persistent or severe joint pain that interferes with your daily activities
- Increased stiffness, especially in the morning or after periods of rest
- Swelling, redness, or warmth around the affected joint
- A grating sensation or bone spurs in the joint
- Reduced range of motion or difficulty moving the affected joint
Preparing for Your Appointment
To make the most of your doctor’s visit, come prepared with the following information:
- A detailed description of your symptoms, including when they started and how they’ve progressed
- A list of any medications, supplements, or therapies you’re currently using
- Any relevant medical history, including previous injuries or conditions
- Questions or concerns you have about your osteoarthritis
Questions Your Doctor May Ask
Your doctor may ask you several questions to better understand your condition, such as:
- When did you first notice your symptoms?
- Have you experienced any recent injuries or trauma to the affected joint?
- How have your symptoms changed over time?
- What treatments or therapies have you tried so far?
Being open and honest with your doctor will help them develop an effective treatment plan tailored to your needs.
Diagnosing Osteoarthritis
To accurately diagnose osteoarthritis, healthcare professionals employ a range of methods, from physical examinations to sophisticated imaging technologies. This comprehensive approach ensures that patients receive an accurate diagnosis, which is crucial for effective treatment planning.
Physical Examination Techniques
A physical examination is a critical component in diagnosing osteoarthritis. Healthcare providers assess joint mobility, look for signs of swelling or tenderness, and evaluate the patient’s range of motion. These techniques help identify the affected joints and the severity of the condition.
X-rays and Magnetic Resonance Imaging
Imaging tests, such as X-rays and Magnetic Resonance Imaging (MRI), play a vital role in diagnosing osteoarthritis. X-rays can reveal joint space narrowing, bone spurs, and other changes associated with osteoarthritis. MRI provides detailed images of the joint, including cartilage, ligaments, and tendons, helping to assess the extent of joint damage.
Joint Fluid Analysis
Joint fluid analysis involves withdrawing fluid from the affected joint to examine for signs of inflammation or infection. This procedure can help rule out other causes of joint pain, such as rheumatoid arthritis or gout.
Ruling Out Other Conditions
Diagnosing osteoarthritis also involves ruling out other conditions that may present similar symptoms. Healthcare providers may conduct additional tests to differentiate osteoarthritis from other types of arthritis or joint disorders.
| Diagnostic Method | Description | Key Findings in Osteoarthritis |
|---|---|---|
| Physical Examination | Assessment of joint mobility and signs of inflammation | Reduced range of motion, tenderness, swelling |
| X-rays | Imaging to visualize joint space and bone changes | Joint space narrowing, bone spurs |
| MRI | Detailed imaging of joint structures | Cartilage loss, ligament or tendon damage |
| Joint Fluid Analysis | Examination of fluid withdrawn from the joint | Signs of inflammation, absence of infection or crystals |
Medication Options for Osteoarthritis
Various medications are available to help manage the symptoms of osteoarthritis, from pain relievers to anti-inflammatory drugs. These medication options can significantly improve the quality of life for individuals living with osteoarthritis.
Over-the-Counter Pain Relievers
Over-the-counter (OTC) pain relievers such as acetaminophen and ibuprofen are commonly used to manage osteoarthritis pain. Acetaminophen is often recommended for mild to moderate pain, while ibuprofen provides additional anti-inflammatory benefits.
Prescription Pain Management
For more severe pain, prescription medications may be necessary. These can include stronger versions of OTC pain relievers or other classes of drugs such as duloxetine, which is used for chronic pain management.
Anti-Inflammatory Drugs
Anti-inflammatory drugs, including both OTC and prescription NSAIDs (Nonsteroidal Anti-Inflammatory Drugs), help reduce inflammation and pain. Examples include naproxen and celecoxib.
Injections for Joint Relief
Corticosteroid injections and hyaluronic acid injections are used to provide relief directly to the affected joint. Corticosteroid injections can reduce inflammation, while hyaluronic acid injections help improve joint lubrication.
| Medication Type | Examples | Primary Use |
|---|---|---|
| OTC Pain Relievers | Acetaminophen, Ibuprofen | Pain relief |
| Prescription Pain Management | Duloxetine, Stronger NSAIDs | Severe pain management |
| Anti-Inflammatory Drugs | Naproxen, Celecoxib | Reduce inflammation and pain |
| Injections | Corticosteroids, Hyaluronic Acid | Direct joint relief |
Physical Therapy and Exercise
Osteoarthritis management often involves a multi-faceted approach, with physical therapy and exercise playing a key role in reducing pain and improving mobility. By incorporating these elements into their treatment plan, individuals can experience significant improvements in their overall quality of life.
Working With a Physical Therapist
A physical therapist can help design a personalized exercise program that addresses specific needs and goals. They can also provide guidance on proper techniques to avoid injury and maximize benefits.
According to the Arthritis Foundation, “Physical therapy can help improve joint mobility, strength, and function, making it easier to perform daily activities.”
Strengthening Exercises for Affected Joints
Strengthening the muscles around the affected joints can help reduce pain and improve function. Examples include:
- Leg lifts for knee osteoarthritis
- Arm curls for elbow or shoulder osteoarthritis
- Wall push-ups for shoulder or upper back osteoarthritis
| Exercise | Benefit |
|---|---|
| Leg Lifts | Strengthens quadriceps, reducing knee pain |
| Arm Curls | Improves elbow flexion and extension strength |
| Wall Push-Ups | Enhances shoulder mobility and strength |
Low-Impact Activities
Low-impact activities such as swimming, cycling, or using an elliptical machine are excellent options for individuals with osteoarthritis. These exercises promote cardiovascular health without putting excessive strain on the joints.
Range of Motion Exercises
Range of motion exercises help maintain or improve joint mobility. Examples include gentle stretching, yoga, or tai chi. These activities can be modified to suit individual needs and abilities.
“Regular exercise and physical therapy can significantly improve the management of osteoarthritis, enhancing both physical function and overall well-being.”
Lifestyle Modifications to Manage Symptoms
Adopting certain lifestyle modifications can significantly help in managing osteoarthritis symptoms. By making a few simple changes, individuals can alleviate pain and improve their quality of life.
Weight Management Strategies
Maintaining a healthy weight is crucial for managing osteoarthritis, particularly in weight-bearing joints like the knees and hips. Losing weight can reduce the strain on these joints, thereby decreasing pain and improving mobility. A combination of a balanced diet and regular exercise can help achieve and maintain a healthy weight.
| Weight Loss Method | Description | Benefits |
|---|---|---|
| Dietary Changes | Eating a balanced diet rich in fruits, vegetables, and whole grains | Reduces inflammation, supports overall health |
| Regular Exercise | Engaging in low-impact activities like swimming or cycling | Improves joint mobility, strengthens surrounding muscles |
Joint Protection Techniques
Protecting joints from further strain is essential for managing osteoarthritis. This can be achieved by using proper body mechanics, avoiding repetitive strain, and utilizing assistive devices when necessary.
“Using the right techniques and tools can significantly reduce the strain on your joints, making daily activities more manageable.”
Heat and Cold Therapy
Applying heat or cold to affected joints can provide relief from pain and stiffness. Heat therapy relaxes muscles and increases blood flow, while cold therapy reduces inflammation and numbs the pain.
Assistive Devices
Utilizing assistive devices such as canes, walkers, or orthotic devices can help reduce strain on joints and improve mobility. These devices can be particularly helpful for individuals with significant joint damage or pain.
By incorporating these lifestyle modifications, individuals with osteoarthritis can better manage their symptoms and improve their overall quality of life.
Complementary and Alternative Treatments
People with osteoarthritis often turn to complementary and alternative treatments to find relief and improve their quality of life. These treatments can be used alongside conventional therapies to manage symptoms more effectively.
Supplements and Nutraceuticals
Some individuals find relief through the use of supplements such as glucosamine and chondroitin, which are believed to support joint health. Other nutraceuticals like omega-3 fatty acids and turmeric have anti-inflammatory properties that may help alleviate osteoarthritis symptoms.
Acupuncture and Massage
Acupuncture involves the insertion of fine needles into specific points on the body to stimulate healing and pain relief. Massage therapy can help reduce stiffness, improve joint mobility, and promote relaxation.
Mind-Body Approaches
Mind-body therapies such as meditation, yoga, and cognitive-behavioral therapy can help individuals manage the emotional and psychological aspects of living with osteoarthritis. These practices promote overall well-being and can enhance pain management strategies.
In conclusion, complementary and alternative treatments offer a variety of options for managing osteoarthritis. It’s essential for individuals to consult with their healthcare provider before starting any new therapies.
Surgical Treatment Options
For those with advanced osteoarthritis, surgery can provide significant relief and improved quality of life. When conservative treatments fail to manage symptoms, surgical interventions become a viable option. The type of surgery recommended depends on the severity of the osteoarthritis, the joints affected, and the patient’s overall health.
Joint Replacement Surgery
Joint replacement surgery, also known as arthroplasty, involves replacing the damaged joint with an artificial one. This procedure is most commonly performed on the hips and knees but can also be done on other joints. Joint replacement surgery can significantly reduce pain and improve function, allowing patients to regain their independence.
| Joint | Success Rate | Recovery Time |
|---|---|---|
| Hip | 95% | 6-12 weeks |
| Knee | 90% | 12-24 weeks |
Arthroscopy Procedures
Arthroscopy is a minimally invasive surgical procedure that allows doctors to look inside the joint using a small camera. During arthroscopy, the surgeon can remove damaged cartilage or bone spurs, and repair ligaments. This procedure is often used for patients with early-stage osteoarthritis or to address specific joint issues.
Osteotomy and Other Surgical Interventions
Osteotomy involves cutting and realigning the bones to relieve pressure on the joint. This procedure is typically considered for younger patients with osteoarthritis who are not yet candidates for joint replacement. Other surgical interventions may include arthrodesis (fusion of the bones) or resection arthroplasty (removal of the damaged joint).
Recovery and Rehabilitation
Recovery and rehabilitation are crucial components of the surgical treatment process. A well-structured rehabilitation program can help patients regain strength, mobility, and function. The specifics of the recovery process vary depending on the type of surgery performed.
Generally, patients can expect a period of physical therapy following surgery, which may include exercises to strengthen the muscles around the joint, improve range of motion, and enhance overall function. Pain management is also a key aspect of the recovery process.
Living Well With Osteoarthritis
Managing osteoarthritis is not just about treating the symptoms; it’s about adopting a holistic approach to improve quality of life. This involves a combination of daily management strategies, making appropriate home modifications, seeking emotional and psychological support, and working closely with your healthcare team.
Daily Management Strategies
Effective daily management of osteoarthritis includes maintaining a healthy weight, engaging in regular exercise such as swimming or cycling, and using assistive devices when necessary. Creating a routine that balances activity with rest is crucial.
Home Modifications for Joint Health
Modifying your home environment can significantly reduce strain on your joints. This can include installing grab bars in strategic locations, using ergonomic furniture, and ensuring that frequently used items are easily accessible.
Emotional and Psychological Support
Living with osteoarthritis can have a significant emotional impact. Seeking support from support groups, engaging in stress-reducing activities like meditation or yoga, and maintaining social connections are vital for emotional well-being.
Working With Your Healthcare Team
A collaborative approach with your healthcare team is essential for managing osteoarthritis effectively. This includes following treatment plans, attending regular check-ups, and communicating openly about your symptoms and any concerns.
Latest Research and Future Treatments
Emerging therapies and regenerative medicine are changing the landscape of osteoarthritis management. Recent studies have focused on developing innovative treatments to alleviate symptoms and potentially reverse joint damage.
Emerging Therapies
Researchers are exploring various emerging therapies, including stem cell therapy and platelet-rich plasma (PRP) therapy. These treatments aim to promote healing and reduce inflammation in affected joints. According to a study published in the Journal of Orthopaedic Research, PRP therapy showed significant improvement in pain and function for patients with knee osteoarthritis.
Regenerative Medicine Approaches
Regenerative medicine approaches, such as cartilage regeneration and tissue engineering, are being investigated for their potential to repair or replace damaged joint tissues. As noted by the American Academy of Orthopaedic Surgeons,
“regenerative medicine holds promise for the future of osteoarthritis treatment.”
American College of Rheumatology Guidelines
The American College of Rheumatology (ACR) regularly updates its guidelines to reflect the latest research and treatment options. Their recommendations include a combination of pharmacologic and non-pharmacologic interventions tailored to individual patient needs.
Conclusion
Osteoarthritis is a complex condition that affects millions of people worldwide. Understanding its symptoms, causes, and treatment options is crucial for effective management. By recognizing the signs of osteoarthritis and seeking medical attention, individuals can take the first step towards alleviating their symptoms and improving their quality of life.
Various treatment options are available, ranging from medication and physical therapy to lifestyle modifications and surgical interventions. A comprehensive approach to osteoarthritis management involves working closely with healthcare professionals to develop a personalized treatment plan. This plan can help individuals manage their symptoms, slow disease progression, and maintain their independence.
By staying informed about the latest research and treatment options, individuals with osteoarthritis can take an active role in their care. Effective osteoarthritis management is key to reducing pain, improving function, and enhancing overall well-being. With the right treatment approach, individuals can navigate the challenges of osteoarthritis and maintain a high quality of life.
FAQ
What is osteoarthritis?
Osteoarthritis is the most common form of arthritis, characterized by the breakdown of cartilage in joints, leading to pain, stiffness, and reduced mobility.
What are the common symptoms of osteoarthritis?
Common symptoms include joint pain and stiffness, reduced range of motion, swelling, tenderness, and a grating sensation in the affected joints.
Which joints are most commonly affected by osteoarthritis?
Osteoarthritis commonly affects weight-bearing joints such as the knees, hips, and spine, as well as the hands and finger joints.
What causes osteoarthritis?
Osteoarthritis is caused by a combination of factors, including age-related wear and tear, genetic predisposition, joint injuries, and obesity.
How is osteoarthritis diagnosed?
Diagnosis involves a physical examination, medical history, imaging tests such as X-rays and MRI, and sometimes joint fluid analysis to rule out other conditions.
What are the treatment options for osteoarthritis?
Treatment options include medications such as pain relievers and anti-inflammatory drugs, physical therapy, lifestyle modifications, and in some cases, surgery like joint replacement.
Can osteoarthritis be cured?
There’s no cure for osteoarthritis, but various treatments can help manage symptoms, slow disease progression, and improve quality of life.
How can I manage osteoarthritis symptoms daily?
Daily management strategies include maintaining a healthy weight, using assistive devices, practicing joint protection techniques, and staying physically active with low-impact exercises.
What lifestyle changes can help alleviate osteoarthritis symptoms?
Lifestyle changes such as weight management, regular exercise, heat and cold therapy, and modifying your home to reduce strain on joints can help alleviate symptoms.
Are there any alternative treatments for osteoarthritis?
Alternative treatments include supplements, acupuncture, massage, and mind-body approaches, which some people find helpful in managing their osteoarthritis symptoms.
When should I consider surgery for osteoarthritis?
Surgery, such as joint replacement, is considered when other treatments have not provided sufficient relief and the condition significantly impacts daily life.
How can I prepare for a doctor’s appointment for osteoarthritis?
Preparing for a doctor’s appointment involves noting your symptoms, medical history, and any questions you have, to discuss with your healthcare provider.