Diabetes mellitus is a chronic condition that can have far-reaching consequences on overall health. When left unmanaged, it can lead to a multitude of complications, affecting various aspects of the body.
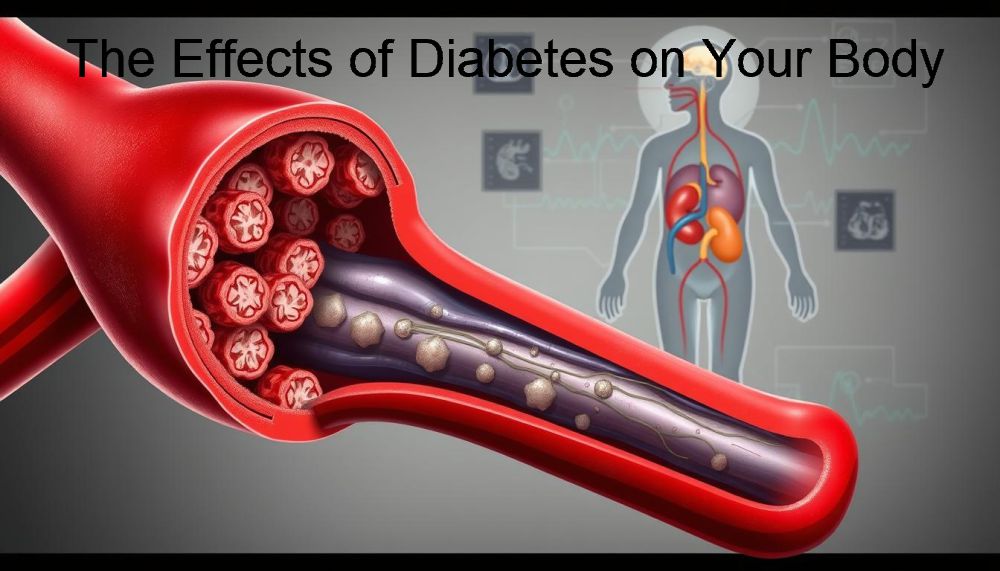
For people with type 2 diabetes, high blood sugar levels can cause damage to organs and systems over time. This can result in serious health issues, making it crucial to manage the condition effectively.
Understanding the impact of diabetes on the body is essential for individuals to take proactive steps towards maintaining their health and preventing long-term damage.
Key Takeaways
- Diabetes mellitus can lead to various health complications if not managed properly.
- High blood sugar levels can cause damage to organs and systems.
- Type 2 diabetes requires careful management to prevent long-term health issues.
- Understanding diabetes is crucial for maintaining overall health.
- Effective management of diabetes can prevent serious health complications.
Understanding Diabetes: Types and Mechanisms
Diabetes mellitus encompasses several distinct types, each with its unique pathophysiology and effects on the body’s ability to regulate blood sugar. Understanding these differences is crucial for effective management and treatment.
Type 1 Diabetes: An Autoimmune Condition
Type 1 diabetes is characterized by an autoimmune response where the body’s immune system attacks and destroys the insulin-producing beta cells in the pancreas. This results in a complete deficiency of insulin production, requiring individuals to rely on insulin therapy to control their blood glucose levels.
How the Immune System Attacks Insulin-Producing Cells
The immune system’s attack on pancreatic beta cells is a complex process involving various immune cells and cytokines. This autoimmune destruction leads to a gradual loss of insulin production, typically presenting in younger individuals.
Type 2 Diabetes: Insulin Resistance
Type 2 diabetes is marked by insulin resistance, where the body’s cells become less responsive to insulin, and over time, the pancreas may also fail to produce enough insulin. This form of diabetes is often associated with lifestyle factors and is the most common type of diabetes.
Progressive Nature of Type 2 Diabetes
Type 2 diabetes is a progressive condition, meaning that over time, the body’s ability to produce insulin can decline further, necessitating more intensive treatment strategies to maintain blood glucose control.
Gestational Diabetes: Temporary but Significant
Gestational diabetes develops during pregnancy, typically in the second or third trimester, due to hormonal changes and insulin resistance. While it usually resolves after pregnancy, it poses risks to both mother and baby and increases the likelihood of developing type 2 diabetes later in life.
How Diabetes Affects Blood Glucose Regulation
Diabetes disrupts the body’s normal regulation of blood glucose levels. In a healthy individual, insulin and glucagon work together to maintain a narrow range of blood glucose. In diabetes, this balance is disrupted, leading to hyperglycemia and potentially serious complications if not managed properly.
The Effects of Diabetes on the Body: An Overview
Diabetes affects the body in numerous ways, from short-term fluctuations in blood sugar to long-term damage to vital organs. Understanding these effects is crucial for managing the condition and preventing complications.
Short-term vs. Long-term Effects
The short-term effects of diabetes are primarily related to fluctuations in blood glucose levels. High blood sugar, or hyperglycemia, can lead to symptoms such as increased thirst and urination, fatigue, and blurred vision. In contrast, low blood sugar, or hypoglycemia, can cause shakiness, dizziness, and even loss of consciousness if not promptly treated.
Long-term effects, on the other hand, result from prolonged exposure to high blood sugar levels, leading to damage to various body systems. This can include cardiovascular disease, kidney damage, nerve damage, and vision problems. As Dr. David M. Nathan, Director of the Diabetes Center at Massachusetts General Hospital, noted,
“The goal of diabetes management is to keep blood glucose levels as close to normal as possible to prevent or delay the onset of complications.”
Risk Factors for Developing Complications
Several risk factors can increase the likelihood of developing diabetes-related complications. These include poor blood sugar control, hypertension, and high cholesterol. Lifestyle factors such as smoking and physical inactivity also play a significant role.
Importance of Blood Sugar Control
Maintaining good blood sugar control is paramount in preventing diabetes complications. This involves regular monitoring of blood glucose levels, adhering to a healthy diet, and engaging in regular physical activity. As emphasized by the American Diabetes Association, “controlling blood sugar is key to managing diabetes and preventing its complications.”
Cardiovascular System: Heart and Blood Vessel Damage
Diabetes can have a profound impact on the cardiovascular system, leading to serious complications. The cardiovascular system, comprising the heart and blood vessels, is crucial for delivering oxygen and nutrients to tissues. Diabetes affects this system in multiple ways, increasing the risk of various cardiovascular diseases.
Increased Risk of Heart Disease and Stroke
Individuals with diabetes are at a higher risk of developing heart disease and experiencing a stroke. Heart disease encompasses conditions that affect the heart’s structure and function, often leading to heart failure or myocardial infarction. The risk of stroke is also elevated due to the potential for blood clots forming in damaged blood vessels. According to the American Heart Association, adults with diabetes are 2-4 times more likely to die from heart disease or experience a stroke compared to those without diabetes.
| Cardiovascular Condition | Risk Factor | Diabetes Impact |
|---|---|---|
| Heart Disease | High Blood Pressure, High Cholesterol | Increased Risk |
| Stroke | Blood Clots, Vessel Damage | Elevated Risk |
| Peripheral Artery Disease | Atherosclerosis | Significant Increase |
How Diabetes Damages Blood Vessel Walls
Diabetes damages blood vessel walls through several mechanisms, affecting both large and small blood vessels. High glucose levels over time can lead to the formation of advanced glycosylation end-products (AGEs), which accumulate in the vessel walls, causing inflammation and damage.
Large and Small Blood Vessel Damage
Large blood vessel damage is associated with atherosclerosis, where plaques form in the arteries, potentially leading to blockages. Small blood vessel damage affects the microvasculature, impairing the exchange of nutrients and waste. This damage can result in various complications, including peripheral artery disease.
“Diabetes is a major risk factor for cardiovascular disease, and the presence of diabetes should be considered when assessing cardiovascular risk.” –
American Diabetes Association
Peripheral Artery Disease in Diabetic Patients
Peripheral artery disease (PAD) is a condition characterized by the narrowing of peripheral arteries due to atherosclerosis. Diabetic patients are at an increased risk of developing PAD, which can lead to pain during walking (claudication), non-healing wounds, and potentially, amputation if left untreated.
Managing diabetes effectively is crucial to mitigating the risk of cardiovascular complications. This includes maintaining good blood glucose control, managing blood pressure and cholesterol levels, and adopting a healthy lifestyle.
Nervous System Complications: Diabetic Neuropathy
Nerve damage, or diabetic neuropathy, is a frequent issue for people with diabetes. Diabetic neuropathy refers to the damage caused to the nerves by high blood sugar levels over time. This condition can affect various aspects of a person’s health, from sensation in the hands and feet to the functioning of internal organs.
The impact of diabetic neuropathy can be widespread, affecting not just the peripheral nerves but also the autonomic and central nervous systems. Understanding the different types of neuropathy and their effects is crucial for managing diabetes effectively.
Peripheral Neuropathy: Damage to Hands and Feet
Peripheral neuropathy is one of the most common forms of diabetic neuropathy. It affects the nerves in the hands and feet, leading to symptoms such as numbness, tingling, and pain. The feet are particularly vulnerable, and peripheral neuropathy can lead to unnoticed injuries, which can become infected and potentially lead to serious complications.
Symptoms and Progression
The symptoms of peripheral neuropathy can vary but often include:
- Numbness or tingling sensations in the hands and feet
- Pain, which can be sharp, dull, or burning
- Increased sensitivity to touch
- Muscle weakness, particularly in the feet
As peripheral neuropathy progresses, it can lead to significant disability and increase the risk of foot ulcers and amputations.
Autonomic Neuropathy: Effects on Internal Organs
Autonomic neuropathy affects the autonomic nervous system, which controls involuntary actions of the body, such as heart rate, digestion, and blood pressure. When diabetes damages these nerves, it can lead to a range of problems, including:
| System Affected | Possible Complications |
|---|---|
| Digestive System | Gastroparesis, constipation, diarrhea |
| Cardiovascular System | Orthostatic hypotension, abnormal heart rate |
| Urinary System | Urinary retention, incontinence |
Central Nervous System Effects
The central nervous system, comprising the brain and spinal cord, can also be affected by diabetes. High blood sugar levels can impair cognitive function and increase the risk of dementia. Additionally, diabetes can lead to an increased risk of stroke and other vascular conditions that affect the brain.
Managing blood glucose levels is crucial to preventing or slowing the progression of these complications. By understanding the risks and taking proactive steps, individuals with diabetes can reduce their risk of developing diabetic neuropathy and its associated complications.
Renal System: Kidney Damage and Disease
One of the significant risks associated with diabetes is the development of kidney disease, which can progress to severe stages if not managed properly. Diabetes can lead to kidney damage over time, affecting the body’s ability to filter waste and regulate fluid balance. This damage can result from high blood sugar levels, which strain the kidneys.
How Diabetes Affects Kidney Function
Diabetes affects kidney function by damaging the tiny blood vessels within the kidneys, impairing their ability to filter waste from the blood effectively. High blood sugar levels can cause the blood vessels to become narrow and weak, reducing blood flow and leading to kidney damage. As a result, the kidneys’ filtering capability is compromised.
Stages of Diabetic Kidney Disease
Diabetic kidney disease progresses through several stages, starting with microalbuminuria, where small amounts of albumin (a protein) are detected in the urine. As the disease advances, it can lead to more severe kidney damage and eventually kidney failure. Monitoring kidney function regularly is crucial for early detection and management.
From Microalbuminuria to Kidney Failure
The progression from microalbuminuria to kidney failure involves several stages, each characterized by increasing kidney damage and decreasing kidney function. Early detection at the microalbuminuria stage allows for interventions that can slow disease progression. Managing blood sugar levels and blood pressure is critical in preventing further kidney damage.
Preventing and Managing Kidney Complications
Preventing and managing kidney complications in diabetes involves maintaining tight control over blood sugar levels and blood pressure. Lifestyle modifications, including a healthy diet and regular exercise, can also help mitigate the risk of kidney damage. Regular monitoring and follow-up with healthcare providers are essential for early detection and effective management of diabetic kidney disease.
Visual System: Eye Complications
Eye health is a critical concern for individuals living with diabetes. Diabetes can lead to several eye complications, potentially resulting in vision loss if not properly managed.
Diabetic Retinopathy: Damage to the Retina
Diabetic retinopathy is a condition where high blood sugar levels damage the blood vessels in the retina, the light-sensitive tissue at the back of the eye. This damage can lead to vision problems and even blindness.
Proliferative vs. Non-proliferative Retinopathy
There are two main types of diabetic retinopathy: non-proliferative and proliferative. Non-proliferative diabetic retinopathy (NPDR) is characterized by the early changes in the retina, including microaneurysms and hemorrhages. Proliferative diabetic retinopathy (PDR) is a more advanced stage, where new, fragile blood vessels grow in the retina, which can lead to severe vision loss.
Cataracts and Glaucoma Risks
Diabetes also increases the risk of developing cataracts and glaucoma. Cataracts involve the clouding of the eye’s lens, while glaucoma damages the optic nerve. Both conditions can lead to vision loss if not treated promptly.
- Cataracts can be treated with surgery.
- Glaucoma treatment often involves medication or surgery to reduce eye pressure.
Protecting Your Vision with Diabetes
To protect your vision, it’s essential to manage your diabetes effectively. This includes:
- Maintaining blood sugar levels within your target range.
- Getting regular eye exams to detect any issues early.
- Managing blood pressure and cholesterol levels.
By taking these steps, you can significantly reduce your risk of developing serious eye complications.
Digestive System: Gastrointestinal Effects
The gastrointestinal effects of diabetes are multifaceted, involving several organs and systems. Diabetes can lead to a variety of digestive issues, ranging from mild discomfort to severe complications.
Gastroparesis: Delayed Stomach Emptying
Gastroparesis is a condition where the stomach takes too long to empty its contents. This can lead to nausea, vomiting, and feeling full after eating only a small amount. Management includes dietary changes and medications to stimulate stomach emptying.
- Eating smaller, more frequent meals
- Avoiding fatty or high-fiber foods
- Using prokinetic agents to enhance gastric motility
Effects on the Liver and Pancreas
Diabetes significantly affects the liver and pancreas. The pancreas is crucial for insulin production, while the liver plays a key role in glucose regulation.
Fatty Liver Disease and Diabetes
Fatty liver disease is common in people with diabetes, particularly those with type 2 diabetes. It occurs when excess fat builds up in the liver, potentially leading to inflammation and scarring. Lifestyle modifications, including weight loss and improved glucose control, are essential for managing fatty liver disease.
Diabetic Diarrhea and Other Digestive Issues
Diabetic diarrhea is a complication that can result from nerve damage (neuropathy) affecting the digestive tract. Other issues include constipation and fecal incontinence. Treating diabetic diarrhea involves managing blood glucose levels, dietary adjustments, and sometimes medication.
- Maintaining tight blood glucose control
- Adjusting diet to include more fiber
- Using antidiarrheal medications as prescribed
Immune System: Compromised Defenses
The immune system of individuals with diabetes is often weakened, making them more prone to various infections. This compromised state is due to the complex interplay between high blood sugar levels, insulin resistance, and the body’s immune response.
Increased Susceptibility to Infections
People with diabetes are more susceptible to infections because their bodies either don’t produce enough insulin or can’t effectively use the insulin they produce. High blood glucose levels over time can lead to damage in various body systems, including the immune system.
Common Infections in People with Diabetes
- Urinary Tract Infections (UTIs): More frequent and severe in people with diabetes.
- Skin Infections: Bacterial and fungal infections are common due to high glucose levels in the skin.
- Fungal Infections: Conditions like candidiasis thrive in high-glucose environments.
| Infection Type | Common Causes | Symptoms |
|---|---|---|
| Urinary Tract Infections | Bacteria (e.g., E. coli) | Burning sensation while urinating, frequent urination |
| Skin Infections | Bacteria (e.g., Staphylococcus), Fungi (e.g., Candida) | Redness, swelling, warmth, and pain in the affected area |
Slow Wound Healing in Diabetic Patients
Diabetes impairs the body’s ability to heal wounds due to factors like neuropathy, reduced blood flow, and compromised immune function. High blood sugar levels can damage the nerves and blood vessels, making it harder for wounds to heal.
Managing diabetes effectively is crucial to preventing infections and promoting wound healing. This includes maintaining good blood sugar control, practicing good hygiene, and seeking medical attention promptly if signs of infection occur.
Skin Complications: Dermatological Effects
Individuals with diabetes are prone to various skin conditions that can significantly impact their quality of life. High blood sugar levels over time can lead to a range of dermatological issues, from mild to severe.
Common Skin Conditions Associated with Diabetes
Diabetes increases the risk of developing certain skin conditions, including bacterial and fungal infections. These infections thrive in high-glucose environments.
Bacterial and Fungal Infections
Bacterial infections such as staphylococcal and streptococcal infections are more common in people with diabetes. Fungal infections, including those caused by Candida, can also occur, often in moist areas of the body.
Diabetic Dermopathy and Other Skin Manifestations
Diabetic dermopathy, characterized by light brown, scaly patches on the skin, is another condition associated with diabetes. Other skin manifestations include necrobiosis lipoidica diabeticorum, a rare condition that causes lesions on the skin, often on the legs.
Managing these skin complications involves maintaining good blood glucose control, practicing good hygiene, and seeking medical attention when necessary.
Sexual and Reproductive Health Impacts
The impact of diabetes on sexual health is multifaceted, affecting both men and women in different ways. Diabetes can lead to a range of sexual and reproductive health issues, making comprehensive management crucial.
Effects on Male Sexual Function
Diabetes can significantly affect male sexual function, primarily through the development of erectile dysfunction. High blood sugar levels over time can damage blood vessels and nerves, impairing the ability to achieve and maintain an erection. Additionally, diabetes can impact testosterone levels, further complicating sexual health.
Erectile Dysfunction and Testosterone Levels
Erectile dysfunction is a common issue among men with diabetes. Managing blood sugar levels and maintaining a healthy lifestyle can help mitigate this condition. Moreover, monitoring and addressing any changes in testosterone levels is vital for overall sexual well-being.
Effects on Female Reproductive Health
Women with diabetes may experience various reproductive health issues, including menstrual irregularities and complications during pregnancy. Diabetes can affect the body’s ability to conceive and carry a pregnancy to term, making careful management of blood glucose levels essential for reproductive health.
Managing Sexual Health with Diabetes
Managing sexual health with diabetes involves a combination of lifestyle modifications, careful blood sugar monitoring, and, when necessary, medical interventions. Open communication with healthcare providers is crucial for addressing sexual health concerns and developing a personalized management plan.
Oral Health: Gum Disease and Dental Problems
The connection between diabetes and oral health is complex and multifaceted. Diabetes can affect oral health in various ways, leading to issues such as gum disease and other dental problems.
The Diabetes-Periodontal Disease Connection
There’s a well-established link between diabetes and periodontal disease. Periodontal disease is a chronic infection of the gums and bone that support the teeth, which can lead to tooth loss if not treated. People with diabetes are more susceptible to periodontal disease due to their compromised ability to fight off infections and heal wounds.
Maintaining Oral Health with Diabetes
Maintaining good oral health is crucial for individuals with diabetes. This involves regular dental check-ups, good oral hygiene practices, and a healthy diet.
Preventive Dental Care Strategies
Some effective strategies for preventive dental care include:
- Brushing teeth at least twice a day with fluoride toothpaste
- Flossing daily to remove plaque and food particles
- Using an antibacterial mouthwash to reduce plaque and gum inflammation
- Visiting the dentist regularly for check-ups and cleanings
| Oral Health Practice | Benefit |
|---|---|
| Regular Brushing | Removes plaque and bacteria |
| Daily Flossing | Prevents gum disease and bad breath |
| Antibacterial Mouthwash | Reduces gum inflammation and plaque |
Mental Health: Psychological Effects of Diabetes
The management of diabetes can lead to various mental health challenges, including depression and anxiety. The constant need to monitor blood glucose levels, manage diet, and maintain an exercise routine can be stressful and overwhelming.
Depression and Anxiety in People with Diabetes
Individuals with diabetes are at a higher risk of developing depression and anxiety due to the chronic nature of the condition. Studies have shown that people with diabetes are more likely to experience these mental health issues compared to the general population.
The Bidirectional Relationship
There is a bidirectional relationship between diabetes and mental health; not only can diabetes contribute to the development of mental health issues, but these issues can also affect diabetes management. For instance, depression can make it more challenging to adhere to a diabetes management plan.
Diabetes Distress and Management Burnout
Diabetes distress, a condition characterized by feelings of frustration and burnout related to diabetes management, is common among individuals with diabetes. This distress can lead to management burnout, where patients feel overwhelmed and less motivated to manage their condition effectively.
- Recognizing the signs of diabetes distress and management burnout is crucial.
- Healthcare providers can offer support and resources to help manage these conditions.
- Lifestyle modifications and stress management techniques can also play a significant role.
By understanding the psychological effects of diabetes and addressing them appropriately, individuals with diabetes can improve their overall well-being and quality of life.
Managing Diabetes to Prevent Complications
To prevent complications, individuals with diabetes must adopt a comprehensive management plan. This involves a combination of medical treatment, lifestyle adjustments, and regular monitoring.
Blood Sugar Monitoring and Control
Monitoring blood glucose levels is fundamental to diabetes management. It helps in understanding how different factors like diet, exercise, and medication affect blood sugar levels.
Target Blood Glucose Levels
Aiming for target blood glucose levels is crucial. Typically, the target is to have a fasting blood glucose level between 80-130 mg/dL and less than 180 mg/dL after meals.
| Time | Target Blood Glucose Level |
|---|---|
| Fasting | 80-130 mg/dL |
| After Meals | Less than 180 mg/dL |
Lifestyle Modifications: Diet, Exercise, and Stress Management
Lifestyle changes play a significant role in managing diabetes. A healthy diet, regular physical activity, and effective stress management can significantly improve blood glucose control.
Diet: Focus on consuming a balanced diet rich in vegetables, fruits, whole grains, and lean proteins. Avoid sugary drinks and foods high in sugar and saturated fats.
Exercise: Regular physical activity, such as walking, can help lower blood glucose levels. Aim for at least 150 minutes of moderate-intensity aerobic exercise per week.
Stress Management: Techniques like meditation, yoga, or deep breathing can help manage stress, which is important because stress can raise blood glucose levels.
Working with Healthcare Providers
Collaboration with healthcare providers is essential for effective diabetes management. Regular check-ups and adjustments to treatment plans as needed can help prevent complications.
By following these strategies, individuals with diabetes can better manage their condition and reduce the risk of complications.
Conclusion: Living Well with Diabetes
Effective diabetes management is crucial for maintaining overall health and preventing complications. By understanding the condition and its effects on the body, individuals can take proactive steps to manage their diabetes.
Living with diabetes requires a multifaceted approach that includes blood glucose control, lifestyle modifications, and regular monitoring. By working closely with healthcare providers, individuals can develop a personalized plan to manage their condition.
Diabetes management is not just about controlling blood sugar levels; it’s about maintaining overall health and well-being. By making informed choices about diet, exercise, and stress management, individuals can reduce their risk of developing complications and improve their quality of life.
With the right tools and support, individuals with diabetes can lead active and fulfilling lives. By prioritizing diabetes management and overall health, individuals can take control of their condition and live well with diabetes.
FAQ
What are the main types of diabetes?
The main types of diabetes are type 1 diabetes, type 2 diabetes, and gestational diabetes. Type 1 diabetes is an autoimmune condition where the immune system attacks insulin-producing cells. Type 2 diabetes is characterized by insulin resistance, where the body becomes less responsive to insulin. Gestational diabetes develops during pregnancy.
How does diabetes affect blood glucose regulation?
Diabetes affects blood glucose regulation by impairing the body’s ability to produce or use insulin effectively. Insulin is a hormone that regulates blood glucose levels. In diabetes, high blood glucose levels can damage various body organs and systems.
What are the short-term and long-term effects of diabetes?
Short-term effects of diabetes include high blood glucose levels, which can cause symptoms like increased thirst and urination. Long-term effects include damage to organs like the kidneys, eyes, and nerves, increasing the risk of complications like heart disease, kidney failure, and vision loss.
How does diabetes damage blood vessels?
Diabetes damages blood vessels by causing high blood glucose levels, which can lead to inflammation and damage to the blood vessel walls. This can increase the risk of cardiovascular disease, including heart attacks and strokes.
What is diabetic neuropathy, and how does it affect the body?
Diabetic neuropathy is a type of nerve damage that occurs in people with diabetes. It can cause symptoms like numbness, tingling, and pain in the hands and feet. Autonomic neuropathy can affect internal organs, while central nervous system effects can impact cognitive function.
How can diabetes be managed to prevent complications?
Diabetes can be managed through blood sugar monitoring and control, lifestyle modifications like diet and exercise, and stress management. Working with healthcare providers is also crucial in managing diabetes effectively.
What are the risks associated with diabetes and cardiovascular disease?
People with diabetes are at increased risk of cardiovascular disease, including heart attacks and strokes. High blood glucose levels can damage blood vessels, increasing this risk.
How does diabetes affect the kidneys?
Diabetes can damage the kidneys by causing high blood glucose levels, which can lead to diabetic kidney disease. This can progress to kidney failure if left unmanaged.
What are the effects of diabetes on the visual system?
Diabetes can cause eye complications like diabetic retinopathy, cataracts, and glaucoma. High blood glucose levels can damage the blood vessels in the retina, leading to vision loss.
How can people with diabetes protect their vision?
People with diabetes can protect their vision by controlling their blood glucose levels, getting regular eye exams, and managing other health conditions like high blood pressure.